Support
Organization
For
Trisomy

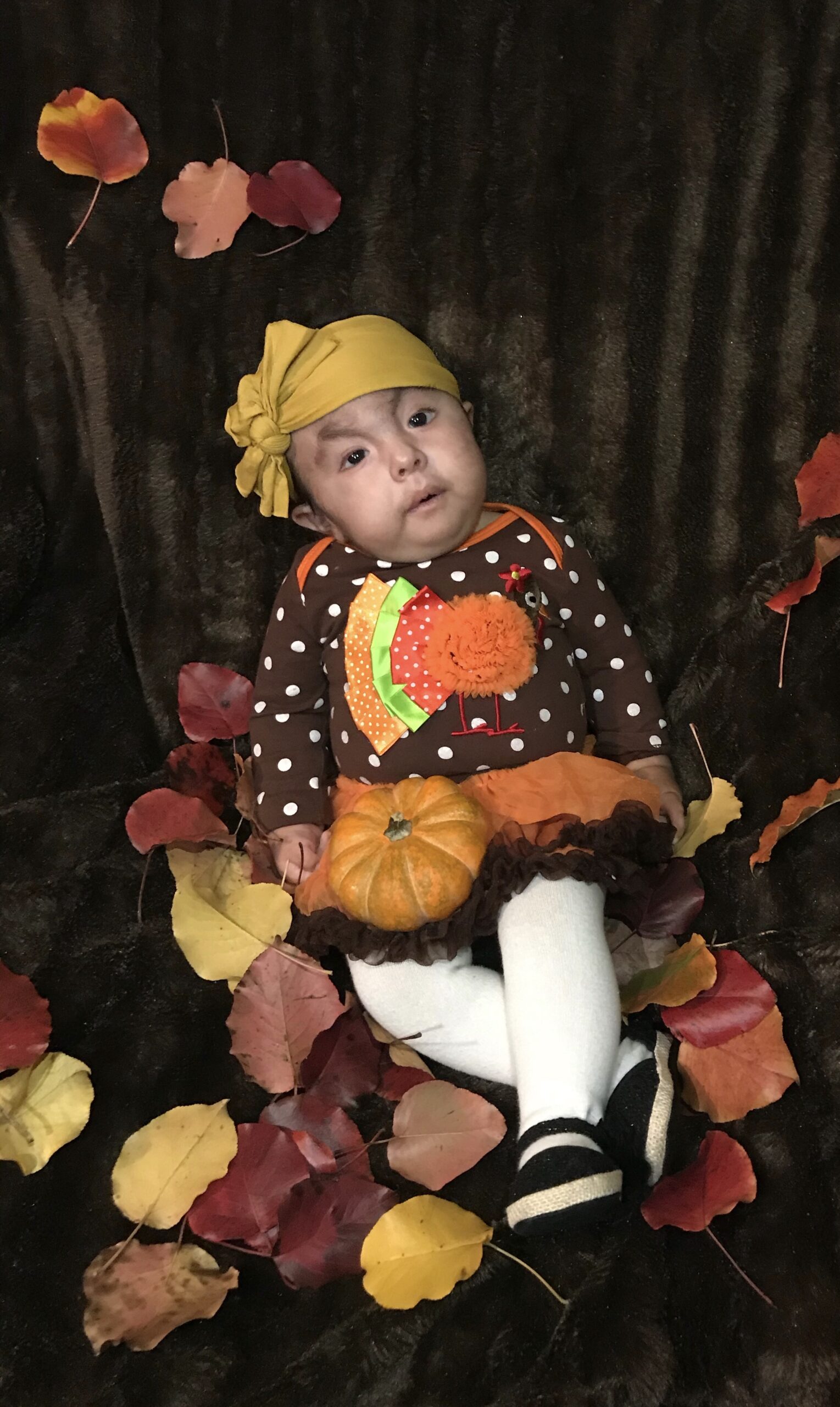
SOFT has been empowering families with children diagnosed with Trisomy 18, 13 and related chromosomal disorders for over 40 years.
WE’RE SO GLAD YOU FOUND US!
How we Support
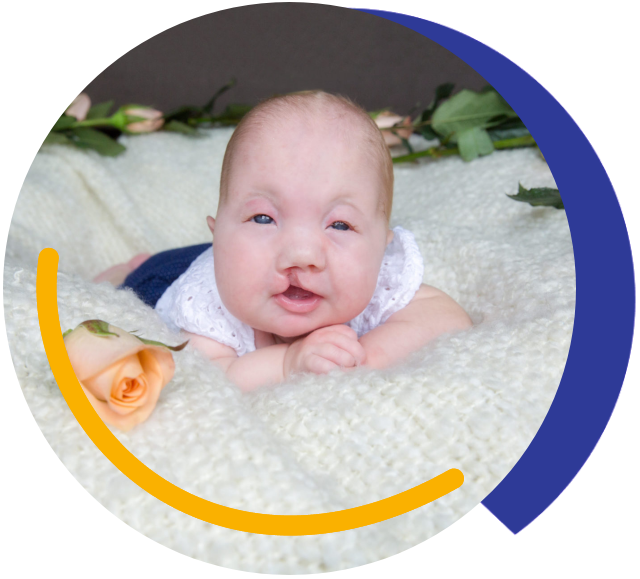

We host an annual conference.

We connect and support families.

We lead the efforts with trisomy awareness month.

We fund medical research.

We partner with medical professionals.



What is SOFT
SOFT is a network of families and professionals dedicated to providing support and understanding to families involved in the issues and decisions surrounding the diagnosis and care in Trisomy 18, 13 and other related chromosomal disorders. Support can be provided during prenatal diagnosis, the child’s life and after the child’s passing. SOFT is committed to respect a family’s personal decision and to the notion of parent-professional relationships.

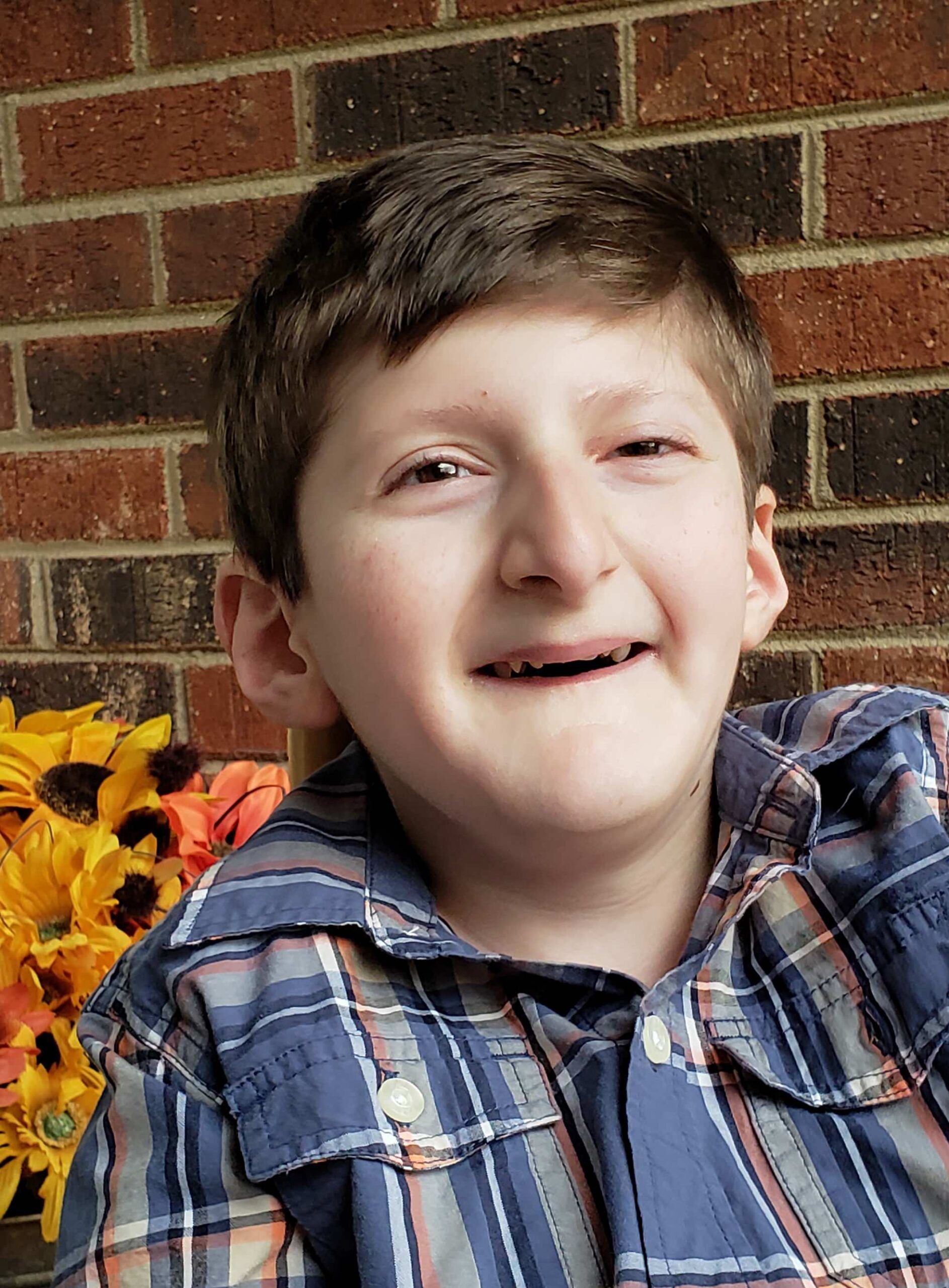

HOW SOFT HELPS FAMILIES

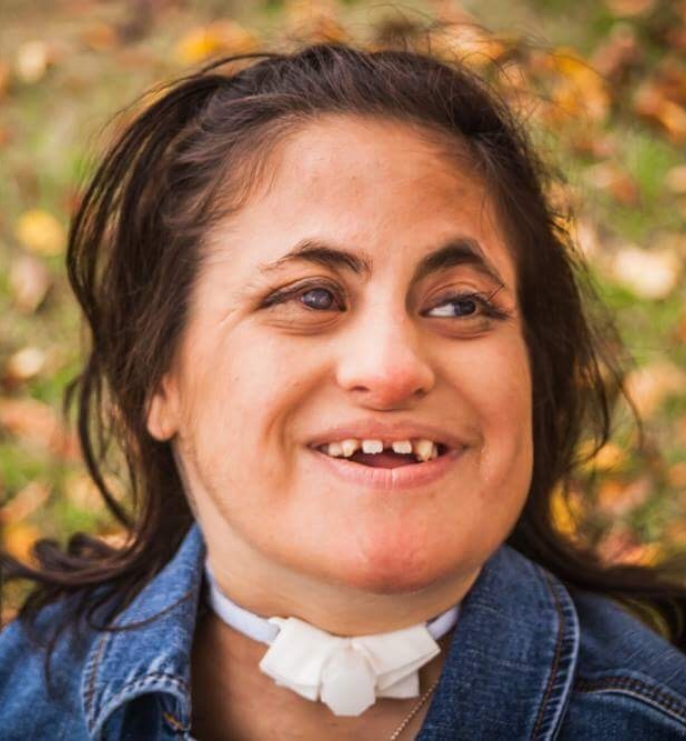

Supportive Network
SOFT provides a support network to connect families with children diagnosed with Trisomy 18, 13 and related chromosomal disorders.
Navigating the Journey
SOFT provides information and resources on Trisomy 18, 13 and related chromosomal disorders, as well as opportunities for connection and community building. Empowers families to navigate their journey with confidence and advocacy for their needs.
Overcoming Challenges
Through the power of togetherness, SOFT helps families overcome the complex and challenging issues related to diagnosis and care. Helping families find hope and positivity in their journey.
OUR MISSION STATEMENT
SOFT inspires hope and respects all on their Trisomy journey.
SOFT MISSION STATEMENT
SOFT inspires hope and respects all on their Trisomy journey.
OUR VALUE STATEMENTS
SOFT values EDUCATION
to empower families and professionals through their Trisomy Journey.
SOFT values and celebrates HOPE
through sharing our stories to celebrate the legacy and value each child brings to their Trisomy Journey.
SOFT values RESEARCH
discovery, and current knowledge of the science of trisomy conditions that lay the foundation of treatment and innovative therapies.
SOFT values our unique COMMUNITY
of families and professionals by promoting a culture of support, respect, and acceptance for all.
SOFT values RESPECT
for each family’s decisions through a culture that regards each child as unique and deserving of dignity.
NOW THAT YOU FOUND US – CONNECT WITH US
WHAT’S THE NEXT STEP?

Contact SOFT
Parents can reach out to SOFT through the website, email, or phone with questions and concerns or to be connected with someone in their area.

Join the Community
We understand the trisomy journey. Connect with other families who are traveling this road today through the SOFT Facebook group or other social media channels.

Access Resources
Parents will have access to information, resources, and ongoing support related to Trisomy 18, 13 and related chromosomal disorders, helping them navigate their journey with confidence and positivity.
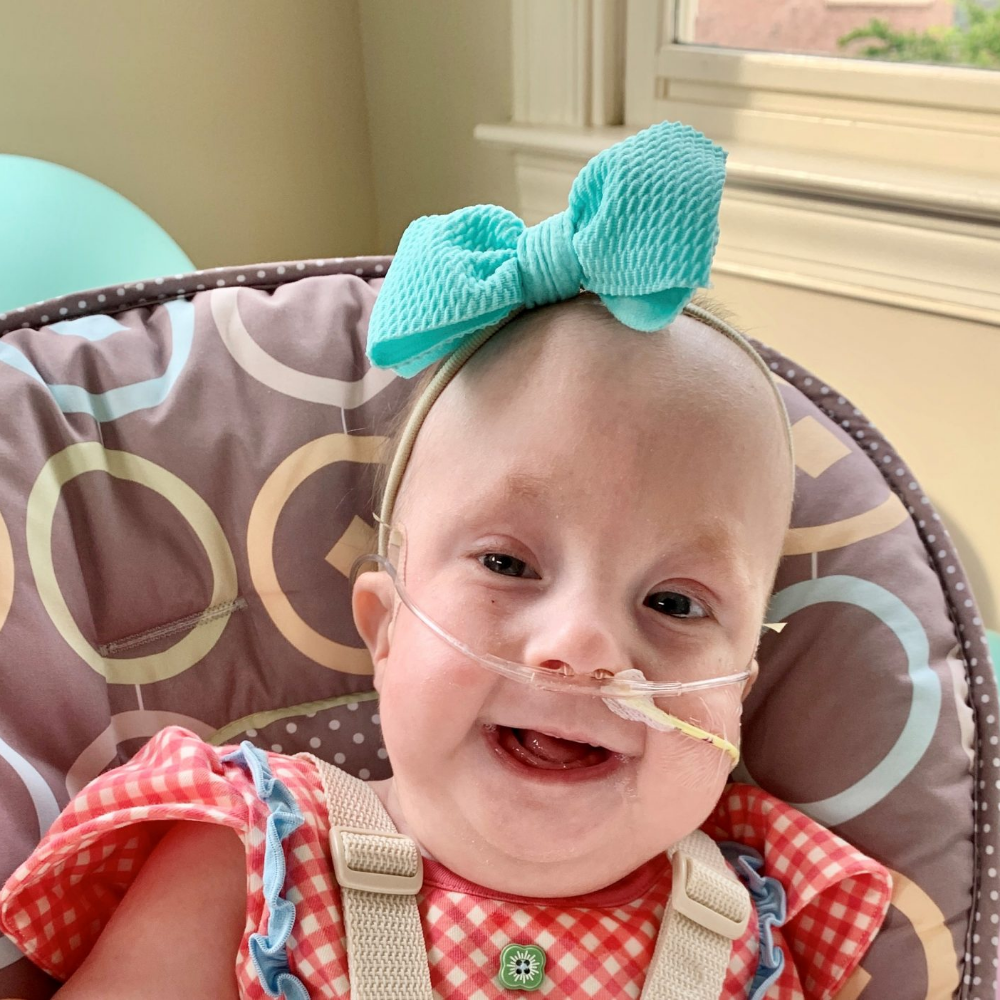



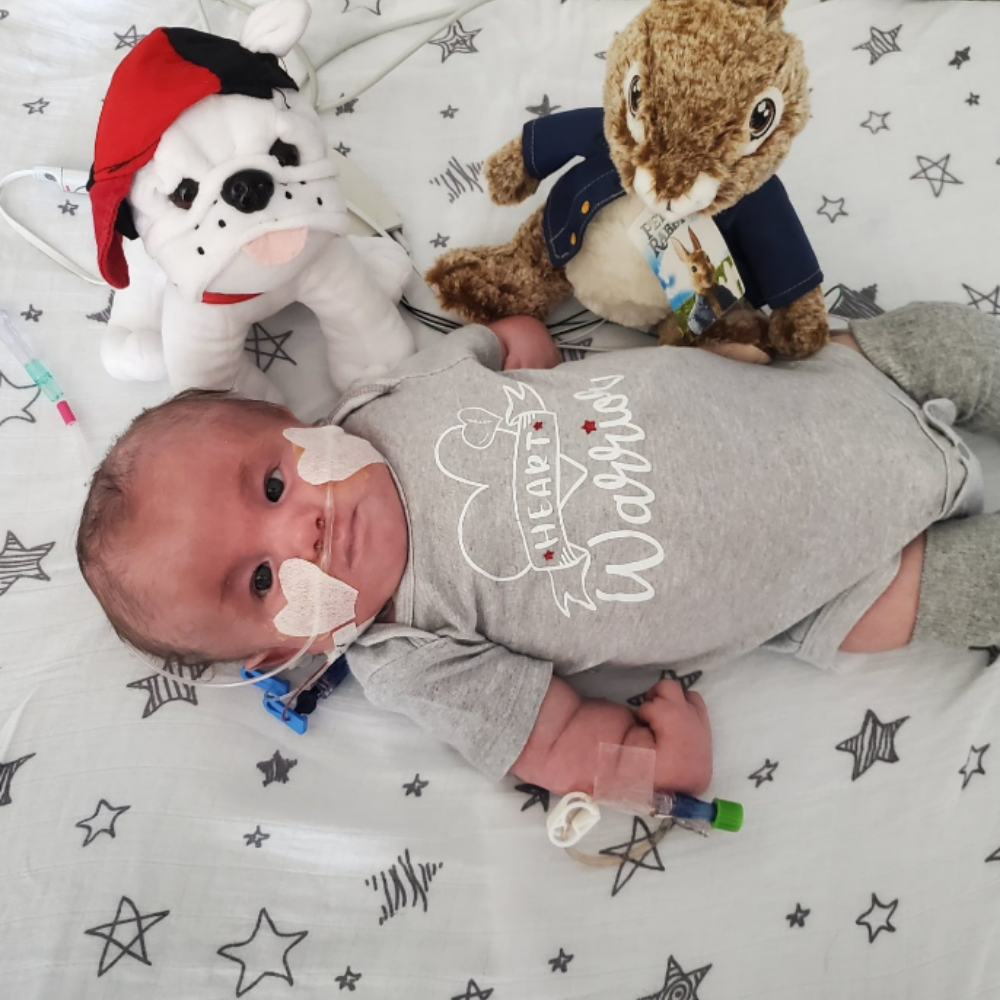
BECOME A MEMBER OF SOFT
CREATE AN ACCOUNT TO CONNECT WITH SOFT
DONATE TODAY
Help support our mission!